Personal Story: Juliet's story: No reconstruction is a post-mastectomy option
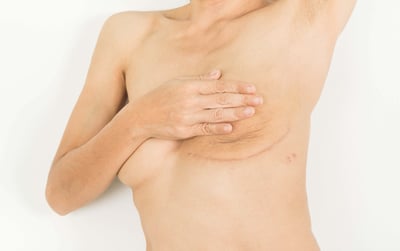
In a March 2018 article from breastcancercare.org, Juliet conveys her personal experience with a breast cancer diagnosis and her decision to not have her breasts reconstructed after her mastectomy. She details the emotional complexity of her thought process and the empowerment she felt in her decisions. (5/24/18)
Contents
| What are the issues and options? | Questions for your doctor |
| What does this mean for me? | Resources |
| Get support |
Whether or not to have reconstruction is a personal choice
In the article, "I felt empowered by choosing not to have a reconstruction," published on March 28, 2018 at breastcancercare.org, Juliet from Hertfordshire, UK describes her decision to forego post-mastectomy breast reconstruction.
Juliet recounts her experiences and emotional decision process from diagnosis of breast cancer through mastectomy, to her eventual decision to forego postsurgical reconstruction of her breasts.
She points out that medical practitioners may hold a preconception that reconstruction is a choice that a patient automatically wants. "Everything was spoken about as though it was the next step in my treatment, as though it was inevitable..." She wrote, “...I knew no different—I didn't know anyone who'd had a reconstruction or even breast cancer, and I had got so used to following what the medical professionals told me to do. I came away thinking, 'OK, I don't want to do this, but it's what I have to do.’”
Juliet emphasizes that these are your choices, that options exist and everyone has to find a fit that works for them. She points out that it is important to take time to make decisions. The shock at diagnosis and discussion of mastectomy can make it difficult for many people to take in their post-mastectomy options. Having reconstruction is a choice, just as having no reconstruction is also a choice. Forgoing reconstruction at the same time as mastectomy need not be a final choice—reconstruction can be done months or years later. The bottom line is that you will likely have ample time to decide what suits you.
What are the issues and options?
Although your diagnosis, treatment and overall health can affect whether or not you have breast reconstruction—as well as when you have it and what options are available to you—most women have multiple post-mastectomy options:
- going flat, with no reconstruction and no prosthetics
- no reconstruction, and using a prosthesis in your clothes that provides a breast-shaped silhouette.
- reconstruction with saline or silicone gel implants (implant-based breast reconstruction or IBBR)
- reconstruction with tissue from another region of your own body (autologous tissue breast reconstruction or ATBR)
- nipple and areolar regions can be surgically reconstructed or simulated by traditional or 3D tattooing. Alternatively, some mastectomies safely preserve the nipple and areola (nipple-sparing mastectomy) depending on the location, size and aggressiveness of the tumor.
A myriad of viewpoints on these options are represented online. Each person needs to consider her own medical history, willingness to undergo additional procedures, the possibility of problems that may require more medical attention, and personal preferences to determine her most suitable and desired choice.
Going flat—having no breast reconstruction and not using prostheses—is an option that many women choose and feel comfortable with. This may reflect not wanting further surgeries, living in an area where reconstruction is unavailable, wanting to delay your decision, or a simply a personal aesthetic choice.
Women who have unilateral mastectomy (one breast removed) may opt to also remove their opposite healthy breast (go flat) or have their missing breast reconstructed and their healthy, unaffected breast lifted, augmented or reduced for improved symmetry. Facing the loss of one breast, for example, Juliet chose to have her other breast also removed and to go flat.
While many women prefer to have immediate reconstruction (at the time of mastectomy), delayed reconstruction (mastectomy and reconstruction performed as separate surgeries) is common, particularly when cancer treatment includes chemotherapy or radiation, which can delay healing after reconstruction.
Various options are taken by many women; you will not be alone whatever your choice is. In a 2014 study, 24.8% of women had immediate reconstruction, 16.8% had delayed reconstruction and 58.2% had no reconstruction. Similarly in a 2017 study, 40% of women had postmastectomy breast reconstruction. Among these women rates were highest (55%) among younger women, ages 35-44, and lowest (17%) among women 65 and older.
Although breast cancer in men accounts for less than 1% of all breast cancers, men also face choices about mastectomy and breast reconstruction. Breast reconstruction in men can include fat grafts or small implants to restore natural body contour or scar reduction. Although the percentage of men choosing reconstruction is significantly lower than among women, the breast reconstruction rates for both genders have been increasing annually.
Moberg and colleagues studied choices and satisfaction with outcomes among carriers who had breast reconstruction. Among patients surveyed, 89.5% underwent implant-based breast reconstruction and 10.5% underwent autologous tissue breast reconstruction. Patients experienced complications within 30 days in 28.65% of cases; 14.6% needed further surgery. The study authors reported that women who had reconstruction with their own tissue rather than implants (ATBR vs IBBR), had greater satisfaction with their reconstructed breasts and overall outcome. Health-related quality of life was similar with either type of reconstruction.
What does this mean for me?
Facing mastectomy is challenging. Take time for emotional processing as well as medical decision making.
Juliet's top tips:
- Take all the time you need
- Ask for advice
- Be true to yourself
Most women have time to research and consider their choices before making their decision about reconstruction. Dealing with the shock of a breast cancer diagnosis and treatment can be difficult to focus on issues that come later like reconstruction and difficult to hear options.
Seek medical advice. Ask your plastic surgeon or other practitioners about options. They will have encountered patients who make a range of choices about reconstruction, nipple-sparing mastectomy, tattooing, or no reconstruction. If you’re undecided about reconstruction, consulting with two or three plastic surgeons can clarify the benefits and limitations of various reconstructive options. Women who have more information and experience more shared decision making with their health care providers report greater satisfaction with their choices, regardless of whether they choose breast reconstruction or not.
Get support from friends and family.
Get support from peers and counselors. FORCE's Peer Navigation Program matches program users with a trained peer who shares their experiences and who can provide support. Gain insight from FORCE members who have gone flat or had reconstruction. FORCE’s annual conference features many sessions on mastectomy with experts who provide information on all the options available post-mastectomy. Our conference after-hours Show & Tell Room offers women who are contemplating mastectomy with or without reconstruction the opportunity to meet and learn in person from women who have had these procedures.
FORCE also has a password-protected post mastectomy photo gallery. This gallery has photos submitted by women and men who have undergone mastectomy with and without reconstruction.
Everyone will undoubtedly have an opinion, but ultimately, the decision whether or not to reconstruct is yours. While being diagnosed with breast cancer is not a choice, decisions about mastectomy and reconstruction are.
Share your thoughts on this XRAYS article by taking our brief survey
Posted 5/24/2018
References
"I felt empowered by choosing not to have a reconstruction." breastcancercare.org. Published March 28, 2018.
The Breast Reconstruction Guidebook by Kathy Steligo
Moberg IO, Bredal I, Schneiger MR, et al. "Complications, risk factors, and patients-reported outcomes after skin-sparing mastectomy followed by breast reconstruction in women with mutations." Journal of Plastic Surgery and Hand Surgery 2108; May 9:1-6.
Miller AM, Steiner CA, Barrett ML, et al. "Statistical brief #228: Breast Reconstruction Surgery for Mastectomy in Hospital Inpatient and Ambulatory Settings, 2009–2014." Agency for Healthcare Research and Quality. Oct. 11, 2017.
Morrow M, Li Y, Alderman AK, et al. "Access to Breast Reconstruction After Mastectomy and Patient Perspectives on Reconstruction Decision Making." JAMA Surgery. 2014; 49(10):1015-1021.
National Cancer Institute. “Breast Reconstruction after Mastectomy.” Feb. 24, 2017.
Disclosure
FORCE receives funding from industry sponsors, including companies that manufacture cancer drugs, tests and devices. All XRAYS articles are written independently of any sponsor and are reviewed by members of our Scientific Advisory Board prior to publication to assure scientific integrity.
- What happens if I choose not to have reconstruction? How long will it take to heal? What will my chest look like?
- Is nipple-sparing mastectomy an option for me? How will it affect reconstruction or the possibility of recurrence or a new diagnosis?
- What are my options for reconstruction? How likely am I to be satisfied with the outcome? What if I am dissatisfied with my result? What complications can occur with reconstruction and how will they be rectified?
- If I choose not to have reconstruction now, can I decide to have reconstruction later? How will delaying reconstruction change my options?
- What non-surgical cosmetic alternatives, like tattooing over my mastectomy scars, are available? What types of prostheses might I consider?
The following studies are related to mastectomy and breast reconstruction.
- NCT05720039: Nipple-Sparing Mastectomy With Immediate Implant-Based Reconstruction for Women With Breast Cancer. This study will compare robotic-assisted nipple-sparing mastectomy (NSM) to standard surgery NSM for women with breast cancer.
- NCT02918474: Decision-Making Tool in Supporting Decision-Making in Contralateral Prophylactic Mastectomy in Patients With Newly Diagnosed Breast Cancer. This trial studies the acceptability and usefulness of a tool that supports decision-making for contralateral prophylactic mastectomy in patients with newly diagnosed breast cancer.
- NCT05020574: Microbiome and Association With Implant Infections. This study is looking at whether people with high amounts of certain types of bacteria are more likely to develop tissue expander-related infections than those with lower amounts of bacteria.
Updated: 05/28/2025
FORCE offers many peer support programs for people with inherited mutations.
- Our Message Boards allow people to connect with others who share their situation. Once registered, you can post on the Diagnosed With Cancer board to connect with other people who have been diagnosed.
- Our Peer Navigation Program will match you with a volunteer who shares your mutation and situation.
- Our moderated, private Facebook group allows you to connect with other community members 24/7.
- Check out our virtual and in-person support meeting calendar.
- Join one of our Zoom community group meetings.
Updated: 09/21/2025
The following resources can help you find a plastic surgeon who specializes in breast reconstruction:
Finding a plastic surgeon
- The American Society of Plastic Surgeons has a searchable Plastic Surgeon Referral Service database.
Other ways to find experts
- Register for the FORCE Message Boards and post on the Find a Specialist board to connect with other people who share your situation.
- The website for The Complete Guide to Breast Reconstruction provides information on Choosing the Right Surgeon.
Updated: 11/20/2023

