Article: Artificial intelligence (AI) may find breast cancer on mammograms sooner
Artificial intelligence (AI) tools may help doctors read mammograms. This assistance may lead to earlier diagnoses of breast cancer. (Posted 9/29/23)
Este artículo está disponible en español.
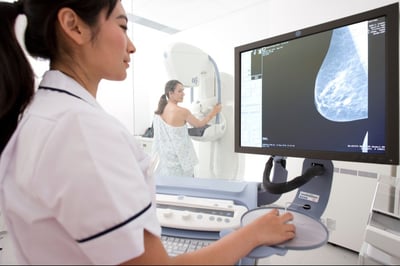
RELEVANCE
Most relevant for: People interested in the use of artificial intelligence in medicine.
It may also be relevant for:
- healthy people with average cancer risk
- people with a family history of cancer
- previvors


Relevance: Medium-High


Research Timeline: Human Research
What is this article about?
This article focuses on a new way radiologists can use artificial intelligence (AI) to improve the interpretation of . AI can spot breast cancer at least as well as humans and often earlier than humans, sometimes up to 5 years earlier. In addition, AI can help general radiologists interpret with the expertise of specialized breast imagers.
Why is this article important?
can find breast cancer before you can feel a lump or notice other symptoms. Doctors look for abnormal changes on a . If an abnormality is seen more tests are ordered to determine whether it is or is not cancer.
Breast cancers that are found early are easier to treat and are often curable. has reduced deaths from breast cancer.
But are not perfect, and they sometimes fail to find cancers. According to the National Cancer Institute, miss 20 percent of breast cancers, and even more in women with dense breast tissue. Doctors who interpret images cannot always see tiny changes, especially when breasts are dense (see our XRAY review on breast density by clicking here). Still, half of people who have yearly at some point have a result—a finding that requires more testing but is then found to be not be cancer.
For these reasons, doctors continue to look for ways to improve the accuracy of . This article focuses on using artificial intelligence (AI) to help read . Studies show that AI can find breast cancers before they are visible to a highly trained human eye.
How does it work?
Typically a is read by one or two radiologists (doctors who specialize in reading x-rays and other images). AI acts as a second “reader,” identifying areas on the image that should be reviewed or imaged more closely. AI technology will soon be able to compare of a person that were taken at different times. This is critical because change is often a sign of cancer. For example, AI might notice a very slight difference between the you had last year and the one you had this year. It would then mark the suspicious area for a doctor to review. AI programs can detect smaller changes that could be missed by the human eye and assist doctors in making a final and more effective diagnosis.
A number of different AI systems are being used in countries around the world, including the United States. A Danish study showed that AI reduced false-positive results by 25 percent. AI does not replace doctors who interpret . Instead, it helps them by reducing their workload and finding cancers they might miss.
In the United States, the Food and Drug Administration () has approved over 20 AI systems for use with . Most AI systems that are approved in the US are designed to work with older, two-dimensional (2D) . Since more than 80 percent of sites that perform in the US use the newer type of 3D (also called digital breast ) the AI systems designed to work with the older are not compatible. Nevertheless, there are AI systems that are currently approved and in clinical use for most systems. In fact, every day more and more breast centers are integrating the use of AI and we expect that will result in improved outcomes and probably the detection of earlier, more curable breast cancers.
What does this mean for me?
The use of AI to read is increasing, both in Europe and in the United States. In the US, multiple AI systems have been approved by the , so clinics are increasingly using AI to assist in the interpretation of
Various clinical trials are underway around the world to help improve the use of AI in reading . These trials are being done to ensure that AI can be used to help read in people of different ages, races and body types. Research is also being done to see whether AI reduces the number of false positives that are not cancer. There are enough breast centers that are using AI that you might consider asking if your breast center has implemented AI.
For women at increased risk there are other imaging tests are recommended in addition to , like . Women at high risk might need annual or in addition to to detect the earliest ,most curable breast cancers. There is AI in development for these imaging approaches as well. Stay tuned for further developments.
References
Satariano A and Metz C, Using A.I. to Detect Breast Cancer That Doctors Miss. The New York Times; published March 5, 2023.
Lauritzen AD, Rodriguez-Ruiz A, von Euler-Chelpin MC, et al. An Artificial Intelligence–based Screening Protocol for Breast Cancer: Outcome and Radiologist Workload. Radiology; 2022; 304; Article number 1. Published online April 19, 2022.
Taylor CR, Monga N, Johnson C, Hawley JR, Patel M. Artificial Intelligence Applications in Breast Imaging: Current Status and Future Directions. Diagnostics. 2023 Jun 13;13(12):2041. Published online June 13, 2023.
National Cancer Institute fact sheet. https://www.cancer.gov/types/breast/mammograms-fact-sheet. Updated February 23, 2023.
Disclosure: FORCE receives funding from industry sponsors, including companies that manufacture cancer drugs, tests and devices. All XRAYS articles are written independently of any sponsor and are reviewed by members of our Scientific Advisory Board prior to publication to assure scientific integrity.
Share your thoughts on this XRAY review by taking our brief survey.
posted 9/29/23
The following are breast cancer screening or prevention studies enrolling people at high risk for breast cancer:
- The Risk Factor Analysis of Hereditary Breast and Ovarian Cancer In Women with , or Mutations. This study seeks to improve researchers’ understanding of how hormonal, reproductive and lifestyle factors may be associated with cancer in high-risk people.
- NCT02620852: Women Informed to Screen Depending on Measures of Risk (WISDOM) study. The goal of this study is to determine whether breast cancer screening can be improved by personalizing each woman’s schedule compared to the current one-size-fits-all annual approach.
Updated: 05/28/2025
The National Comprehensive Cancer Network (NCCN) provides breast cancer risk-management guidelines for people with and mutations. We recommend that you speak with a genetics expert who can review your personal and family history of cancer and help you to determine the best risk management plan. Note that our use of "men" and "women" refers to the sex you were assigned at birth.
Recommended screening for women with mutations:
- Beginning at age 18, be aware of how your breasts normally look and feel. Tell your doctor about any breast changes.
- Beginning at age 25, have a doctor examine your breasts every 6-12 months.
- Beginning at age 25, have an annual breast with contrast (or if is unavailable).
- Beginning at age 30 and continuing until age 75, have an annual and an annual breast with contrast.
- After age 75, speak with your doctor about the benefits and risks of screening.
Risk reduction for women:
- Speak with your doctor about the advantages and disadvantages of risk-reducing mastectomy.
- Research shows that risk-reducing mastectomy can lower the chance of developing breast cancer in high-risk women by about 90 percent. Mastectomy has not been shown to help high-risk women live longer.
- Because some breast tissue remains after mastectomy, some breast cancer risk also remains.
- Speak with your doctor about the benefits and risks of tamoxifen or other estrogen-blocking drugs to reduce your breast cancer risk. The benefits and risks may be different for women with or mutations. Research on the benefit of these drugs to reduce breast cancer risk in women with mutations has been mixed.
Risk management for men:
- Beginning at age 35, learn how to do breast self-exams to check for breast changes.
- Beginning at age 35, have a doctor examine your chest every 12 months.
- Beginning at age 50, consider an annual (especially for men with mutations).
Updated: 06/21/2024
The National Comprehensive Cancer Network (NCCN) provides guidelines for management of breast cancer risk in people with inherited mutations linked to breast cancer. We recommend that you speak with a genetics expert who can look at your personal and family history of cancer and help you determine the best risk management plan.
or
- Beginning at age 40 (or earlier based on your family history of breast cancer)
- recommend yearly
- Beginning at age 30-35
- consider yearly with and without contrast
, or
- Beginning at age 40 (or earlier based on family history):
- recommend yearly
- consider yearly breast with and without contrast
- No specific breast cancer screening guidelines. Risk management should be based on your family history of cancer.
- Beginning at age 30 (or earlier based on family history):
- recommend yearly
- consider yearly breast with contrast
- discuss risk-reducing mastectomy
- Beginning at age 30 (or earlier based on family history):
- recommend yearly
- recommend yearly breast with and without contrast
- discuss risk-reducing mastectomy with your doctor
PTEN
- Beginning at age 18, learn to be aware of changes in breasts.
- Beginning at age 25:
- clinical breast exam every 6-12 months beginning at age 25 or 10 years earlier than the youngest age of onset in the family
- Beginning at age 30:
- yearly and breast with contrast beginning at age 30 or earlier based on the youngest breast cancer in the family
- discuss risk-reducing mastectomy with your doctor
- After age 75
- discuss benefits and limitations of continued screening with your doctor
STK11
- Beginning at age 30:
- clinical breast examination by a health care provider every 6 months starting at age 30
- recommend yearly
- recommend yearly with and without contrast
- discuss risk-reducing mastectomy with your doctor
TP53
- Beginning at age 18, learn to be aware of changes in your breasts.
- Beginning at age 20:
- clinical breast examination by a healthcare provider every 6 months
- recommend yearly breast with and without contrast beginning at age 20 or at the age of earliest breast cancer diagnosis if there is a history of breast cancer before age 20 in family
- Beginning at age 30
- recommend yearly
- Consider risk reducing mastectomy.
- After age 75
- discuss benefits and limitations of continued screening with your doctor
Updated: 12/17/2023
Share your thoughts!
How helpful was this XRAY review? We’d love to hear your feedback in our brief survey.