by Sue Friedman (FORCE) with Janine Guglielmino (LBBC)
When people are diagnosed with cancer, doctors perform tests to learn more about the cancer and the best way to treat it. Ongoing advances in medicine are making it possible for doctors to look at the unique makeup of each patient and their tumor to choose the best medicine for each patient. Though not yet fully realized, these advances are part of a growing field known as “precision medicine” (also sometimes referred to as “personalized medicine”). Precision medicine aims to deliver the right screening, prevention, or treatment options at the right time to achieve the best medical outcome. Precision medicine can improve treatment by helping doctors select treatments that are more effective or lead to fewer side effects, and can help patients in their medical decision making.

With support from Foundation Medicine, Living Beyond Breast Cancer (LBBC) and Facing Our Risk of Cancer Empowered (FORCE) have teamed up on a project to increase knowledge and awareness of precision medicine in breast cancer.
We began this project with a survey for people diagnosed with breast cancer to assess the gaps in knowledge about precision medicine. We surveyed breast cancer patients about their understanding of three types of tests that help guide treatment decisions: pathology, tumor testing and genetic testing for inherited mutations. The survey was open from November 27, 2018 to February 7, 2019. This is the first of several articles that share the results. Over the next few months, we will post additional results and resources to help people diagnosed with breast cancer understand how precision medicine may affect their care.
Who Responded to Our Survey
Our survey received responses from 648 people. Most of the 421 people who answered the question about gender were women; five were male. Men have breast tissue and can develop breast cancer, although their risk is much lower than women’s—less than 1 percent of all breast cancers occur in men.
Geographic location
The majority of survey participants were from the United States, and most states were represented. Seventy-six international respondents responded from Australia, Bangladesh, Canada, France, Germany, Italy, Mexico, the Philippines, Singapore, South Africa, the United Arab Emirates and the United Kingdom.
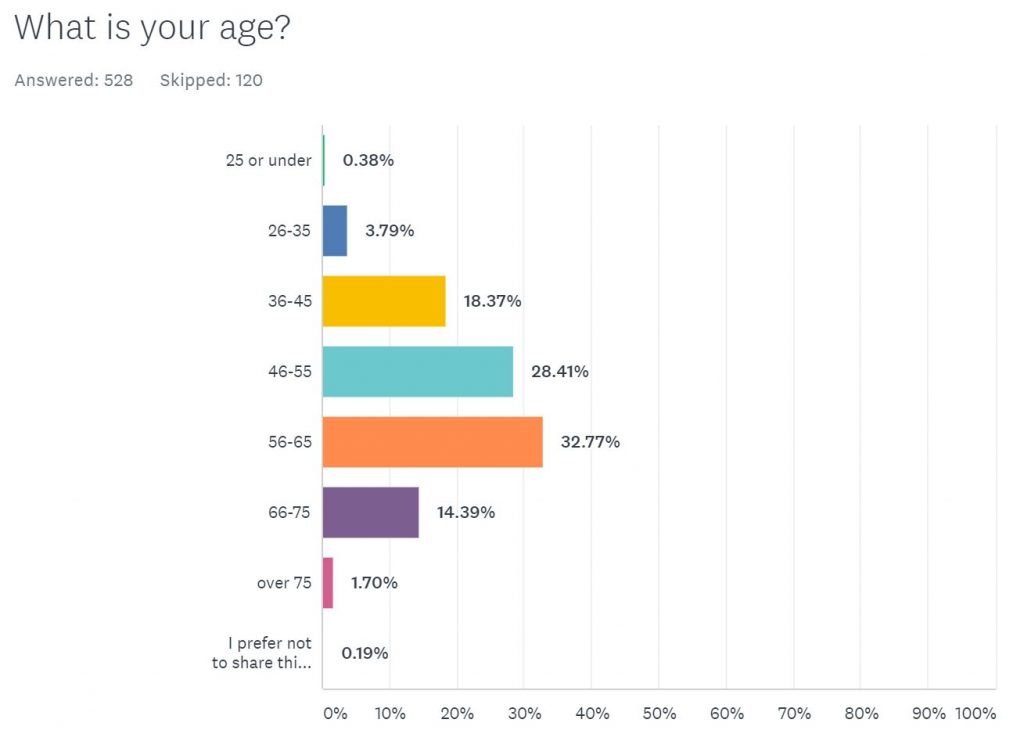
Age
528 people responded to the question about age:
Underserved populations and social determinants of health
We asked participants to indicate if they belonged to any of the categories below, which are communities that are more likely to experience barriers to health care.
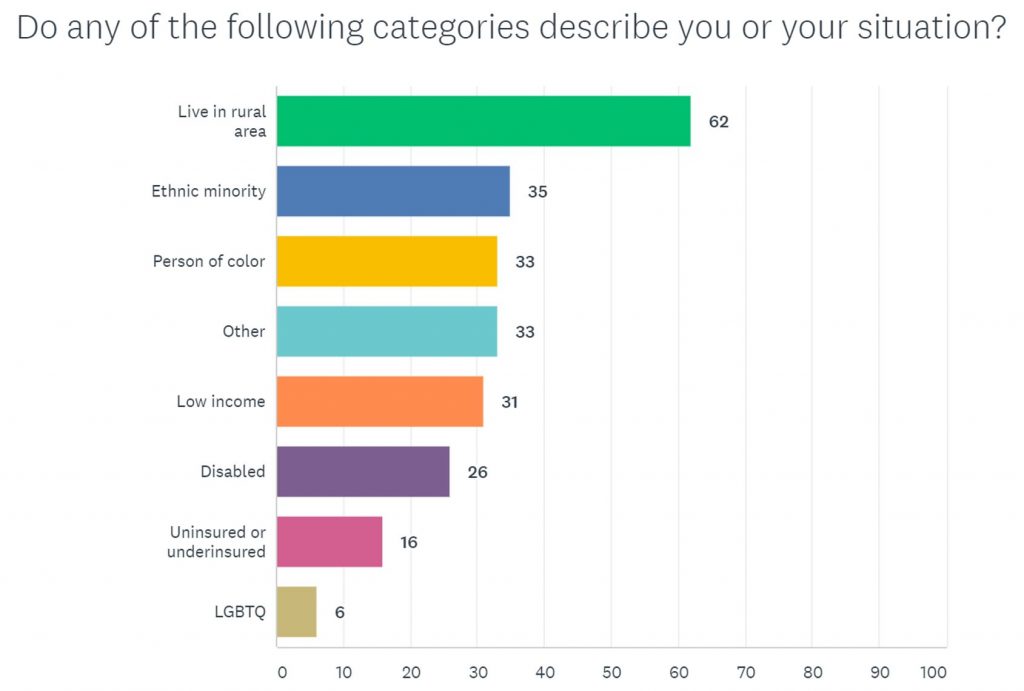
Respondents’
comments about barriers to care included:
“I lost my insurance during treatment.”
“My care is a full-time job and I'm limited in what I can do, due to pain.”
“I had to take early retirement and could not find other work. Lost insurance. Was able to get access to care through Medicaid.”
“I’m a single parent working freelance, so currently without an income while undergoing treatment.”
“I have to travel 140 miles round trip to get cancer care. It takes a whole day to visit the cancer center. I come home exhausted.”
Type and stage of breast cancer
We asked respondents about their type of breast cancer. Most people knew their breast cancer type, especially their hormone and Her2-neu status:
- Hormone receptor-positive (estrogen and/or
progesterone): 56.6% (323) - Triple-negative: 23.3% (133)
- Her2-neu positive: 15.4% (88)
- I’m not sure: 2.3% (13)
Most people also knew their cancer stage.
Replies of the 570 people who responded to this question were:
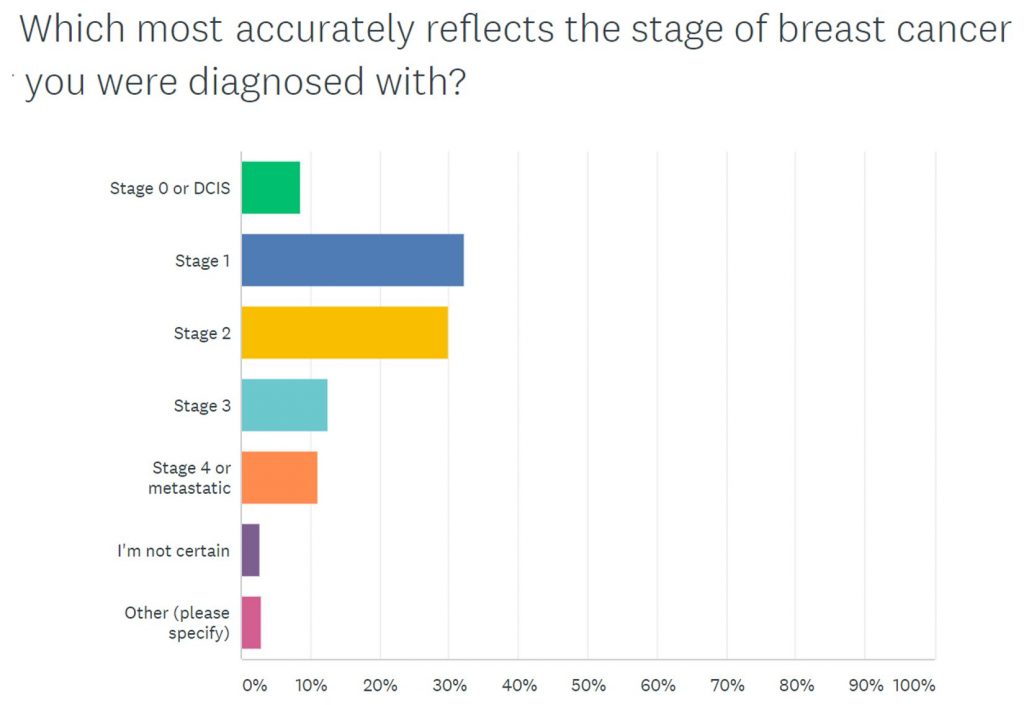
It is important for patients to know the stage and type of their breast cancer, as this information significantly affects which medical options are available.
Pathology Report
The pathology report is the part of an individual’s medical record that describes the tissue that was removed during biopsy or cancer surgery. We asked respondents if they saw or received a copy of their pathology report describing their tumor. Of 556 respondents, the majority said they had seen or received a copy of their report. Almost 7 percent received their pathology report only after requesting it. Ten percent of respondents never received a copy.
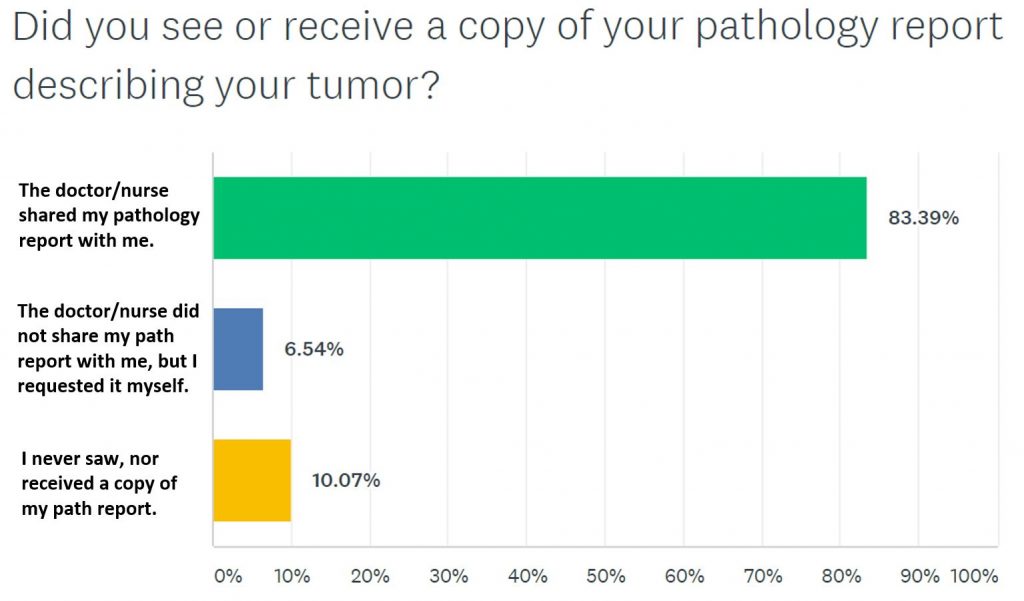
Most people said that their health care provider explained the pathology report to them, and most fully understood their results. Although many people did additional research to better understand their pathology, 14 percent of respondents disagreed or strongly disagreed with the statement “I fully understood my pathology report.”
Every person has a right to see and obtain a copy of their pathology report. Access to medical records is important and can help patients:
- understand their cancer type
- discuss options with their health care
provider - ask questions and clarify things they don’t
understand - get a second opinion
- make informed decisions
- share information with relatives
- search for clinical trials
- understand which tests were ordered and why
Eight people commented that they received their pathology report and other medical records directly through their hospital’s patient portal. Providing patients with online access to their electronic health records (also known as EHR) is becoming more common.
In our survey, people who saw their pathology report were more likely to do additional research and more likely to understand the meaning of the report.
Participants’ thoughts about their pathology report included:
“It was a lot of information to take in at a stressful time.”
“I did not understand any of it despite asking on more than one occasion.”
Tumor Testing
In addition to tumor pathology, sometimes additional tests are run on tumors to provide more information about the cancer and guide treatment decisions. These tests can help doctors personalize a patient’s treatment plan based on unique traits of the cancer. We asked participants to share their knowledge about additional testing of their tumor. We asked about two main types of breast cancer tumor tests:
- Prognostic tests measure risk for cancer recurrence in patients with early-stage cancers. They are used to predict which patients are most likely to benefit from chemotherapy. Almost one-quarter of respondents indicated they had a prognostic test. Examples of these tests include Oncotype DX, MammaPrint, Prosigna and others.
- Biomarker tests look for specific tumor biomarkers to guide treatment – usually in patients with advanced cancers. Some cancer treatments (known as “targeted therapies”) work best on tumors that contain a specific biomarker. Biomarker tests can help doctors select patients who will benefit from a targeted therapy. Tests which are FDA approved to select patients for a specific treatment are sometimes called “companion diagnostic tests.” Examples of biomarker tests include FoundationOne, MSK-Impact, Ventana PD-L1, and others.
Almost one-quarter of respondents indicated that they had one of these tests. Sixty percent of respondents indicated that their doctor explained their tumor test results to them, and 54 percent stated that they fully understood the results. Similar to responses about pathology results, about 1 of 10 respondents stated that they did not fully understand the results of their tumor tests. Most patients did additional research to understand their tumor test results. Of respondents who had prognostic tumor testing, most (86 percent) indicated that their tumor test results influenced their treatment decisions. Almost three-quarters of the people who had biomarker tests said that the results influenced their treatment decisions. Sixty percent of respondents indicated that their doctor explained their tumor test results to them, and 54 percent stated that they fully understood the results. Similar to the responses on pathology results, about 1 of 10 respondents stated that they did not fully understand the results of their tumor tests. Most patients performed their own research to understand their tumor test results. Of respondents who had prognostic tumor testing, most (86 percent) indicated that their tumor test results affected their treatment. Almost three-quarters of the people who had biomarker tests said that the results affected their treatment.
Respondents’ comments about their experience with tumor testing included:
“Sequencing brought a possible immunotherapy clinical trial due to ‘tumor mutational burden.’”
“I do not understand who qualifies for treatment with a targeted therapy.”
“The Drs indicated that testing did affect my treatment, but I still didn't understand all of it.”
“My oncologist did not want to run the Oncotype test so it was not ordered in time to make treatment decisions, however I wanted the results even after treatment had started and I'm glad I asked for it because we found out my tumor had parts that were triple negative, which made me more confident in choosing a more aggressive approach.”
“I wish there was a ‘dictionary’ for all common tumor mutations that was accessible to patients both in terms of getting it and in terms of understanding it.”
Genetic Testing for an Inherited Mutation
Genetic testing for inherited gene mutations involves testing blood or saliva to look for gene changes that increase the risk for developing certain types of cancer. Mutations in BRCA1 and BRCA2 are the most common gene changes associated with breast cancer. Mutations in other genes, including ATM, PALB, CHEK2 and PTEN, can also increase the risk for breast cancer. A higher-than-expected number of survey respondents—more than 80 percent—indicated that they had been tested for an inherited mutation. Among those who participated, 68 percent of LBBC respondents had genetic testing, while 92 percent of FORCE respondents had genetic testing, which is higher than we would expect to see in an unselected population of breast cancer patients. These high numbers may be due to both organizations providing education programs on genetic testing for breast cancer.
A little more than 10 percent of respondents had a genetic test result known as a Variant of Uncertain Significance (VUS). VUS results are called “inconclusive” because experts are uncertain if these changes affect cancer risk.
Here is a summary of the results from respondents who underwent genetic testing. We broke out the responses by organization, due to the large differences between the two groups.
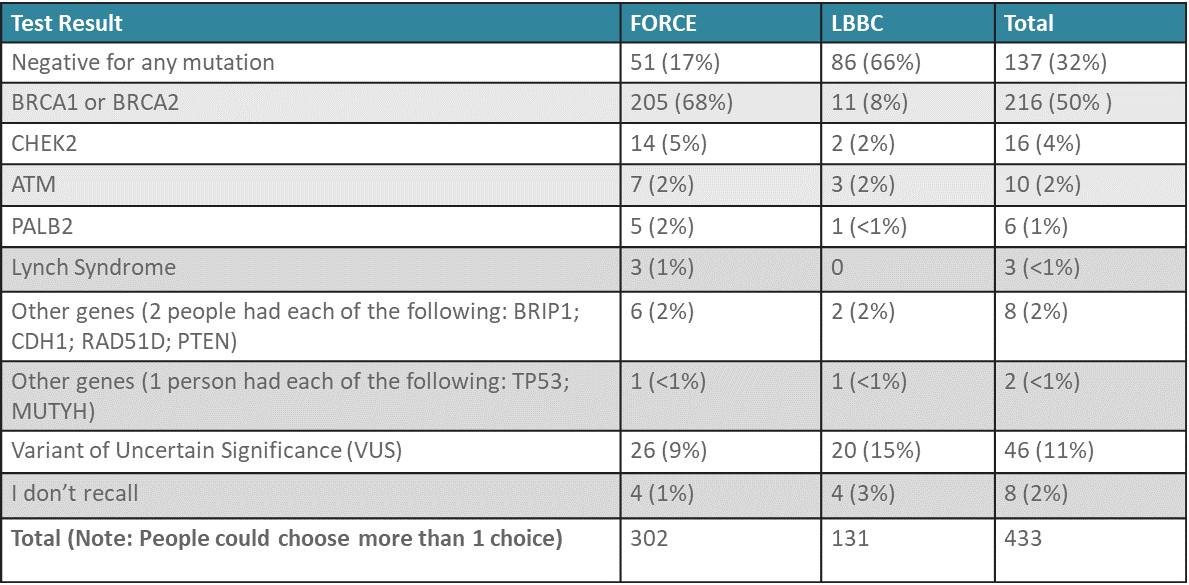
More than 90 percent of respondents said that their health care provider explained their genetic test results, and 85 percent said that they fully understood their results. For most people, genetic test results affected their treatment or surgery decisions. Respondents provided these comments:
“I am now on a PARP inhibitor.”
“I felt comfortable moving forward with breast-conserving surgery, which is what I wanted.”
“Testing positive changed my treatment course dramatically. I went from lumpectomy with radiation to bilateral mastectomy and chemo.”
We asked respondents about any aspects of their genetic test results that they did not understand. Many expressed frustration or confusion about receiving an inconclusive VUS result.
“I do not know what to do next after receiving "VUS." What about my daughter, son, and nieces?”
“I don’t understand the variant of uncertain significance. No one can tell me anything.”
“I have now had four primary cancers. I am wondering whether genetic testing could help me to remain healthy and avoid another diagnosis.”
National guidelines recommend counseling with a genetics expert before and after genetic testing. This is important whether test results are positive, negative, or inconclusive. In each case, a genetics expert can ensure that the results are properly interpreted, discuss medical options, and explain what the results may mean for relatives.
Differences in Knowledge About
Pathology, Tumor Testing and Genetic Testing
Although most patients understood their test results, there were differences in responses between the three types of tests.
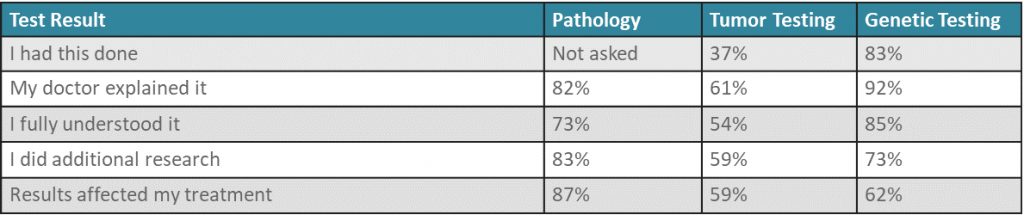
Of the three types of tests in our survey, patients seemed to understand genetic testing the most and tumor testing the least. Almost half of the patients reported that they did not understand their tumor test results. Tumor testing is relatively new compared with pathology and genetic testing, which may contribute to the differences in provider explanation and patient understanding of these tests.
Some respondents expressed confusion about the difference between genetic testing for inherited mutations (also known as “germline mutations” and tumor testing for mutations only found in the tumor (also known as “somatic mutations”). One respondent stated:
“Some people talk about the TUMOR having a BRCA mutation, vs. the WOMAN having a BRCA mutation. I still don't get that.”
As part of our joint project, we will be creating additional resources to help people understand their cancer diagnosis, test results and medical options.
Precision Medicine Terminology
We asked survey respondents how familiar they were with medical terms related to precision medicine, as this is key to understanding the meaning of test results. Several people noted that they had a hard time understanding medical jargon.
For each of the terms below, the definition can be found in the FORCE Glossary.
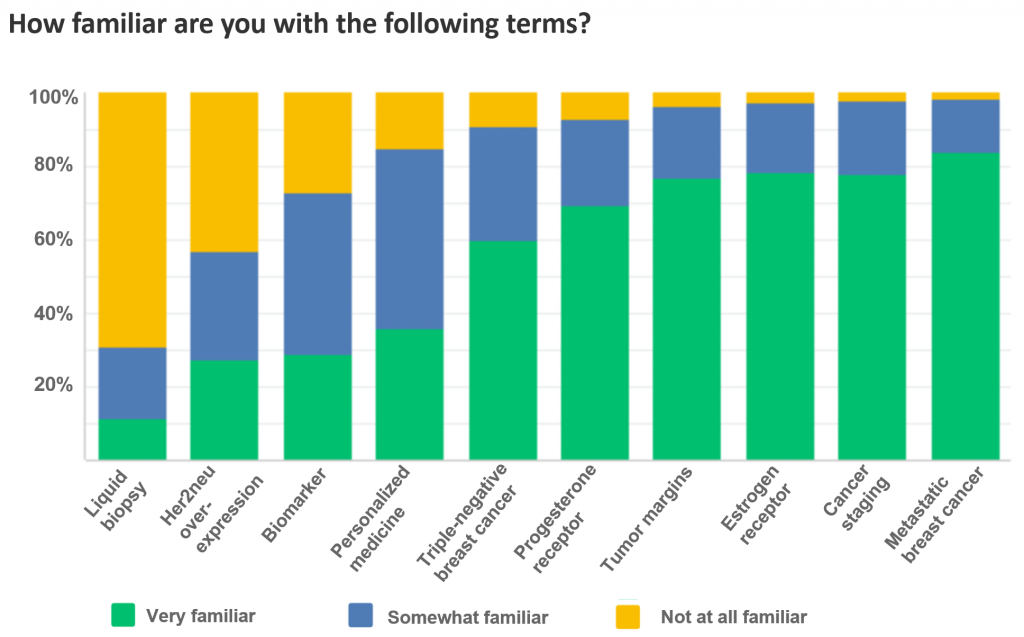
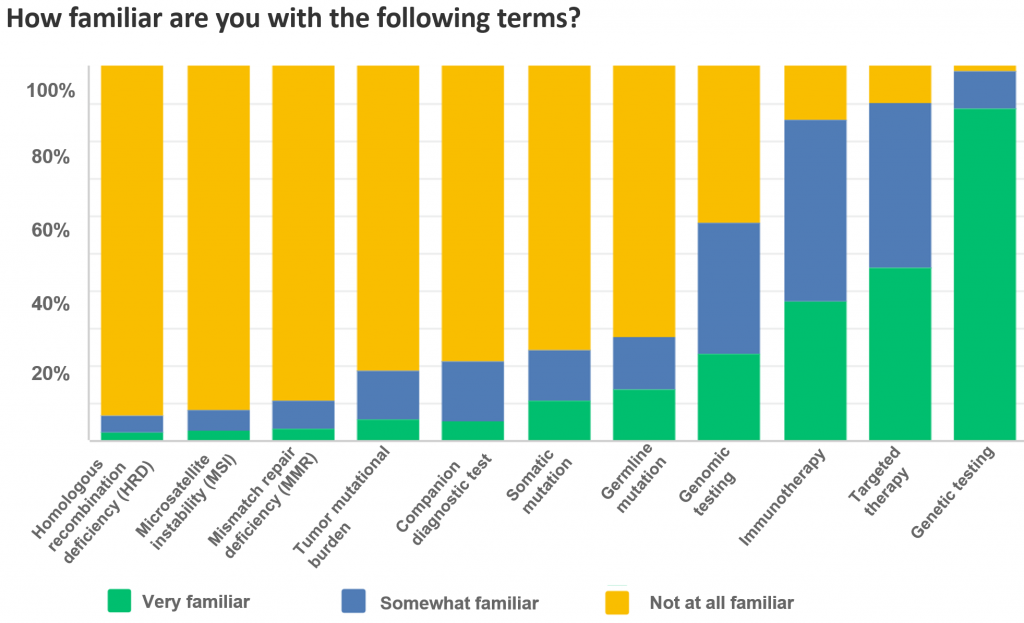
In the words of one respondent:
“I don’t understand the jargon.”
We will address challenges in language and terminology related to precision medicine in future articles.
Final thoughts
These survey results highlight important gaps in patient care and information. For example, one out of 10 respondents indicated that they never saw their pathology report. In the words of one patient:
“After taking this survey, I realize I have not been thoroughly educated about my options or my cancer.”
The FORCE/LBBC collaboration will provide tools and resources to help patients access their medical reports, discuss results with their doctors and take an active role in their treatment plan. Stay tuned!